Conventional methods used in cancer diagnosis of malignant tissues are labour-intensive and time consuming. Cancer surgeons at times, have to send tissue samples to different pathology labs for diagnosis, whose results may take hours or days. This results in a delay in decision-making and therapy. Furthermore, the currently used method for tissue diagnosis known as frozen section analysis, which involves cutting, freezing and staining a tissue sample is a fairly lengthy process and can sometimes give inaccurate results.
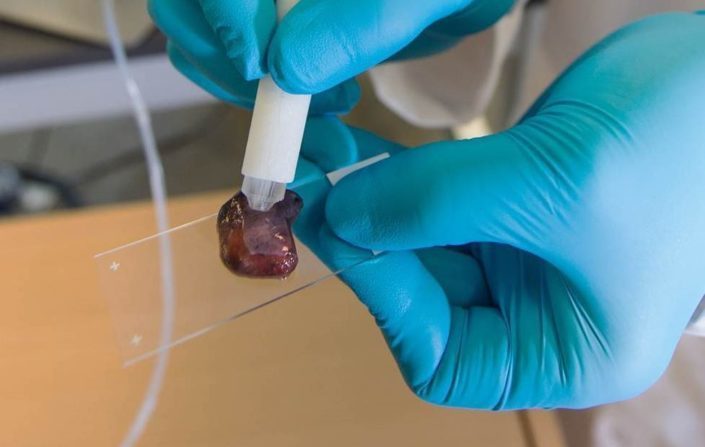
Fortunately, the scientists at the University of Texas-Austin, have developed a new technology called the “MasSpec pen” which uses mass spectrometry to analyse tissues. The handheld instrument is simple by itself, a pen as one might see, which is connected to a large complex machine, a mass spectrometer. How it works is, the pen is held up against a tissue sample suspected of being cancerous. A small drop of water is ejected from the tip of the pen, onto the tissue sample. Any loose molecules present on the tissue enter the water droplet, which is sucked back into the pen. This sample is then sent to the connected mass spectrometer which analyses and determines whether the tissue sample is healthy or cancerous. Detecting cancer is possible due to the distinct molecular “fingerprint” present in malignant tissues.
Photo source: University of Texas at Austin
The researchers have tested the cancer diagnosis device on 253 human tissue samples of breast, lung, thyroid, and ovarian cancer, as well as healthy tissue with an accuracy of 96%. The pen also has the potential to be used in cancer treatment as its tip is 3D-printed using surgical-ready plastic. Doctors can use the pen to ensure every last remnant of cancer tissue is removed, before the patient is closed up, eliminating the need to send more samples to a lab to see if they got it all, and lowering the risk of relapse.
“If you talk to cancer patients after surgery, one of the first things many will say is ‘I hope the surgeon got all the cancer out.’ It’s just heart-breaking when that’s not the case,” says study leader Livia Eberlin. “Our technology could vastly improve the odds that surgeons really do remove every last trace of cancer during surgery.”
An illustration of the MasSpec pen and the instrument, called a mass spectrometer that analyses the tissue. Illustration: University of Texas at Austin
The MasSpec pen technology still has room for improvement as, though the pen is small, it’s just one part of the whole system. The mass spectrometer that the pen feeds is still just as big as the legacy models, and can take up a lot of space in the operating area. However, researchers have already begun testing on smaller models. Before the pen is adopted, it needs to be tested on more tissue samples, as well as during actual surgeries in clinical trials. It also needs to be approved by the US Food and Drug Administration. However, the researchers of this study are optimistic about the mass spectrometry system for detecting cancer and hope to start testing the MasSpec pen in actual surgeries next year.
References:
- Zhang, J., Rector, J., Lin, J. Q., Young, J. H., Sans, M., Katta, N., & Liu, J. (2017). Nondestructive tissue analysis for ex vivo and in vivo cancer diagnosis using a handheld mass spectrometry system. Science Translational Medicine, 9(406), eaan3968.
- https://www.theverge.com/2017/9/7/16267368/masspec-pen-cancer-surgery-device
- https://www.medicalnewstoday.com/articles/319331.php