Male infertility is a medical condition wherein the male is unable to conceive a child. While infertility can occur in both males and females, about 35% of cases of infertility are attributed to male infertility. Male infertility can occur due to a wide range of reasons, but biological aging can be a major contributing factor. Aging is a natural process that occurs over a period of time and leads to a gradual reduction in the robustness of body functions. As the body ages, the function of the testes also gradually deteriorates and eventually, errors start creeping into the highly regulated process of sperm production (also known as spermatogenesis). The two hormones, testosterone, and oestrogen are strong links between aging and reduction in testicular function. As aging progresses, the levels of these hormones reduce, which leads to errors in the spermatogenesis. Ultimately, this cascade leads to the production of low-quality sperm, and thus male infertility.
In June 2019, Jeremy, Gurusubramanian and Vikas Roy, of the Department of Zoology, Mizoram University, published a study in The Journal of Steroid Biochemistry and Molecular Biology, which explored the role of Vitamin D3 in the mitigation of testicular activity by regulating steroidogenesis in aged rats. The study was conducted using rat models that were artificially aged using a chemical called D-galactose. Previous studies have demonstrated the presence of molecular receptors for Vitamin D in the testes, mature sperms and areas of the male ejaculatory tract. This, combined with evidence proving that the lack of Vitamin D severely affects the quality of sperms in both humans and rodents, strongly suggests that Vitamin D plays a pivotal role in regulating male infertility. The main aim of Dr. Roy and his teams’ work was to investigate if Vitamin D could mitigate the loss of age-related testicular function by studying its effect on spermatogenesis and steroidogenesis in D-gal induced aged rats. This work is a first of its kind as previous studies focused on the role of Vitamin D in the alleviation of bone and muscle disorders. The role of Vitamin D in ameliorating male infertility is an unexplored territory.
The following flowchart provides a simplified view of the experimental design of the teams’ work. To summarize, they tried to investigate the effect of Vitamin D on the expression of hormones, steroidogenic markers, and steroidogenic receptors.
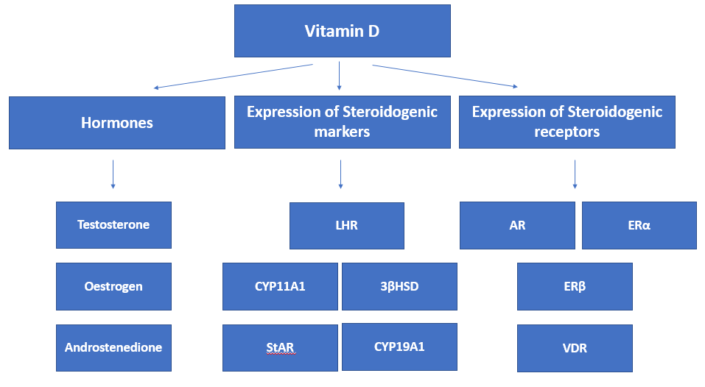
The outcomes of the study elegantly confirm the ability of Vitamin D3 to counter the effects of aging on fertility parameters in male rodents. Let us look at the findings of the study in brief detail:
Vitamin D3 can improve the quantity of daily sperm production
The team was able to find that as the rats aged, the testes of the rats underwent severe deterioration (Panel A in the below image). The administration of Vitamin D showed a marked improvement in the testicular structure (Panel B in the below image), with an increase in the sperm count and daily sperm production.
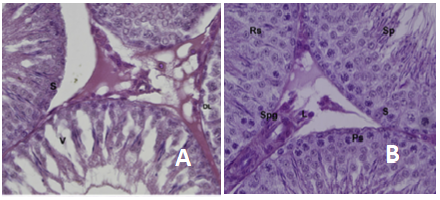
A: Aged testis with high levels of deterioration
B: Histological section of the testis from an aged rat treated with a high-dose of Vitamin D
Vitamin D3 improves the production of testicular steroidogenesis
Aging is associated with a sharp reduction in the production of the steroid hormones – testosterone, androstenedione and oestrogen. The scientists were able to confirm that the administration of Vitamin D successfully increased the production of these hormones in aged rats. To understand how Vitamin D was able to modulate the production of these hormones, they tried to find out if Vitamin D was regulating the production of some precursors to the hormones (which will be referred to as “markers”). The following diagram shows the relationship between steroid hormones and their respective markers.
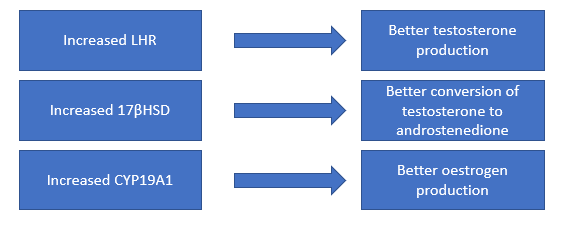
It was seen that Vitamin D successfully elevated the levels of LHR and 17βHSD, thus explaining the improvement in the production of testosterone and androstenedione.
The researchers also analyzed the expression of the receptors for these testicular hormones and they found that Vitamin D3 was able to regulate the levels of the hormones through an interplay between the androgen receptor, oestrogen receptor, and the Vitamin D receptor.
Role of oestrogen
The scientists were able to demonstrate an increase in the levels of the enzyme CYP19A1 in aged rat testes treated with Vitamin D3. Since CYP19A1 is a key enzyme involved in oestrogen production, it is safe to say that Vitamin D increases the production of oestrogen in aged rat testis. Surprisingly, the serum levels of CYP19A1 was reduced by the administration of Vitamin D, thus indicating a low oestrogen level in the serum. This remarkable finding led the team to conclude that Vitamin D3 is able to modulate the relative expression of CYP19A1, and thus oestrogen, in the serum and testes to improve spermatogenesis and alleviate the age-related loss of male fertility.
In conclusion, Dr. Roy and his colleagues explain that Vitamin D3 has a very important role to play in protecting the testes from age-related deterioration. It regulates the production of testicular steroid hormones and steroid receptors. Vitamin D3 treatment can thus be considered as a valid effective form of treatment of male infertility. It can also be a valuable diagnostic tool to confirm male infertility. Dr. Roy confirms that the team is continuing this work to explore other avenues of Vitamin D3 mediated mitigation of male infertility.
References:
- https://rmanetwork.com/blog/male-infertility-cases-and-statistics/
- https://medlineplus.gov/maleinfertility.html
- https://www.ncbi.nlm.nih.gov/pubmed/30923019